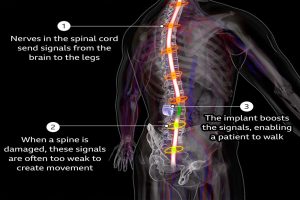
Understanding Atherosclerosis: Its Impact, Development, and Advanced Treatment Strategies
Atherosclerosis is a chronic disease that predominantly affects the arteries. The condition instigates a prolonged inflammatory reaction within the arterial walls, characterized by the accumulation of cholesterol and fatty proteins. Over time, this buildup may calcify, narrowing the diameter of the vessels and obstructing blood flow distally. The plaque formed can also act as a site for platelet attraction, potentially causing emboli to dislodge and travel distally. In some instances, plaque fissuring occurs, leading to the formation of fresh clots that can block the vessel.
Atherosclerosis
The clinical importance of atherosclerosis and its consequences depend on the specific vessels affected. If atherosclerosis manifests in the carotid artery, small emboli may develop and result in a stroke. In the heart, plaque fissuring could cause an acute vessel thrombosis, leading to a myocardial infarction, or heart attack. In the legs, chronic vessel narrowing may limit a patient’s ability to walk and eventually cause distal ischemia and gangrene of the toes.
The pathophysiology of atherosclerosis is complex and involves multiple interconnected systems, including oxidative stress, dysfunctional endothelium, diseased lipid uptake, cell apoptosis, thrombotic and pro-inflammatory responses, and alterations in smooth muscle cells (SMCs). These processes contribute to plaque growth, making them key targets in the treatment of atherosclerosis. Over the past few decades, numerous scientific studies and clinical practices have focused on targeting these processes to improve atherosclerosis outcomes. Stent, balloon, and nanoparticle-based delivery strategies have been developed to ensure therapeutic effect and lesion homing delivery.
Recently, liposomes have emerged as a promising tool in both the diagnosis and management of atherosclerotic cardiovascular disease (ASCVD). Liposomes can function as contrast agents for imaging techniques, as delivery vehicles for antiatherosclerotic drugs, genes, and cells to established plaque sites, and as vaccine adjuvants against atherosclerosis mediators. This approach has the potential to enhance visualization of early atherosclerotic lesions and improve residual ASCVD risk management.
One of the most significant risk factors in the development of atherosclerosis and subsequent cardiovascular disease is hypercholesterolemia. Strategies that effectively reduce low-density lipoprotein (LDL) levels have been shown to decrease cardiovascular events in both primary and secondary prevention across different patient groups. Statins, in particular, have demonstrated substantial improvement in the prognosis for reducing atherosclerotic heart disease and are often the treatment of choice for reducing LDL. However, despite their efficacy, a residual cardiovascular risk remains in many patients, necessitating alternative or additional treatments.
Ezetimibe is one such alternative for statin-intolerant patients, and it can also be added to statins for a more comprehensive approach. However, even in combined statin and ezetimibe therapy, some patients still present with elevated LDL levels and cardiovascular risk. This has led to the identification of additional effective and safe lipid-lowering strategies, such as proprotein convertase subtilisin kexin type 9 (PCSK9) inhibitors. These inhibitors are clinically available as alirocumab and evolocumab and have shown significant lowering of LDL-C, non-high-density lipoprotein cholesterol, and lipoprotein(a) levels. They can be used as monotherapy or in combination with other lipid-lowering drugs and have demonstrated a favorable impact on atherosclerotic plaque progression and the lipidic profile of patients. Importantly, PCSK9 inhibitors do not adversely affect glucose metabolism and do not increase the incidence of new-onset diabetes mellitus.
Long-term studies with PCSK9 inhibitors, particularly evolocumab, have shown sustained LDL-C reduction without evidence of safety concerns. The FOURIER trial, for instance, analyzed the outcome of 27,564 patients with atherosclerotic cardiovascular disease and LDL-C >70 mg/dl who were receiving statin (±ezetimibe) therapy and were randomly assigned to receive evolocumab or a matching placebo. With evolocumab, LDL-C was quickly and significantly reduced, with the median LDL-C level at around 30 mg/dl. Furthermore, the primary endpoint—a composite of cardiovascular death, myocardial infarction, stroke, hospitalization for unstable angina, or coronary revascularization—was reduced with evolocumab compared to the placebo group. These results were primarily driven by reductions in myocardial infarction, stroke, and coronary revascularization, demonstrating the potential of PCSK9 inhibitors in atherosclerosis treatment.
While the study and understanding of atherosclerosis have advanced significantly over the years, further research is needed to refine and develop new treatment strategies and to better understand the full implications of existing ones. By continuing to delve into the complex pathophysiology of this disease and its treatment, we can better manage its impact and improve patient outcomes.