Atherosclerosis: An In-depth Look at the Silent Killer
Atherosclerosis, a common yet serious condition, is a disease that primarily affects the arteries, the vessels that carry oxygen-rich blood from the heart to the rest of the body. The disease is characterized by a chronic inflammatory reaction within the walls of the arteries, where deposits of cholesterol and fatty proteins, known as plaques, accumulate over time. This article aims to provide a comprehensive understanding of atherosclerosis, from its pathophysiology to its potential life-threatening consequences and the latest advancements in its management.
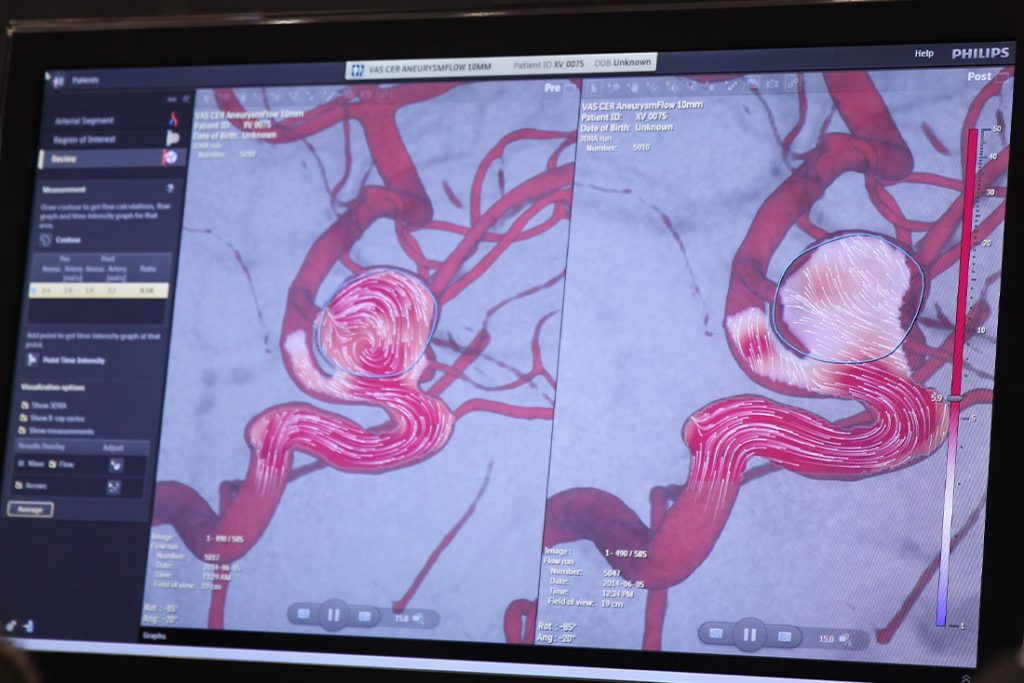
Atherosclerosis
Understanding Atherosclerosis: The Pathophysiology
The development of atherosclerosis is a complex process that begins when the innermost layer of the artery, the endothelium, becomes damaged. This damage may be triggered by various risk factors, including high blood pressure, smoking, high cholesterol, and diabetes.
Once the endothelium is damaged, cholesterol and other fatty substances in the blood can seep into the arterial wall, triggering an immune response. White blood cells are dispatched to engulf the cholesterol, leading to the formation of plaques – fatty deposits within the arterial wall. Over time, these plaques grow and harden, a process known as calcification, which can reduce the diameter of the vessel and impede blood flow to tissues and organs downstream.
Notably, these plaques are not just passive obstructions in the vessels. They may serve as sites for the aggregation of platelets, the blood cells responsible for clotting. These platelets can form a clot, or thrombus, on the plaque’s surface, which may break off and block blood flow at a site distal to the plaque, a process known as embolization. Furthermore, the plaque itself can rupture, or fissure, exposing its core to the blood stream and leading to the rapid formation of a clot that can completely occlude the vessel.
The Impact of Atherosclerosis: From Silent Progression to Catastrophic Events
The clinical significance of atherosclerosis largely depends on which artery or arteries are affected. For example, when atherosclerosis occurs in the carotid arteries, which supply blood to the brain, small emboli may break off and block smaller brain arteries, leading to a stroke.
In the coronary arteries, which supply blood to the heart muscle, plaque rupture can lead to the formation of a clot that blocks blood flow to a part of the heart, causing a myocardial infarction, or heart attack. This is one of the most dangerous complications of atherosclerosis and is a leading cause of death worldwide.
In the lower extremities, atherosclerosis can lead to peripheral artery disease. Chronic narrowing of these vessels can restrict blood flow to the muscles during activity, causing a condition called claudication, which is characterized by leg pain or fatigue while walking. In severe cases, restricted blood flow can lead to tissue death or gangrene, which may necessitate amputation.
Diagnosis, Management, and Treatment of Atherosclerosis
The diagnosis of atherosclerosis involves a thorough medical history, physical examination, and various diagnostic tests. These tests may include blood tests to measure cholesterol levels, imaging tests to visualize the arteries, and functional tests to assess the effect of atherosclerosis on heart or brain function.
Managing atherosclerosis typically involves lifestyle modifications such as a heart-healthy diet, regular exercise, smoking cessation, and weight control. Medications may also be used to lower cholesterol levels, reduce blood pressure, prevent clot formation, or manage symptoms such as chest pain.











