Understanding Skeletal Age Determination: A Crucial Tool in Modern Medicine
This article discusses skeletal age determination, a crucial tool in modern medicine. It covers the process of skeletal maturation, the methodology used for determining skeletal age, and the various factors that can influence this process. The article also explores the significance of skeletal age determination in diagnosing certain diseases, where there may be a discrepancy between the individual’s chronological age and their skeletal age. Finally, it underscores the value of this practice in both clinical and legal contexts.
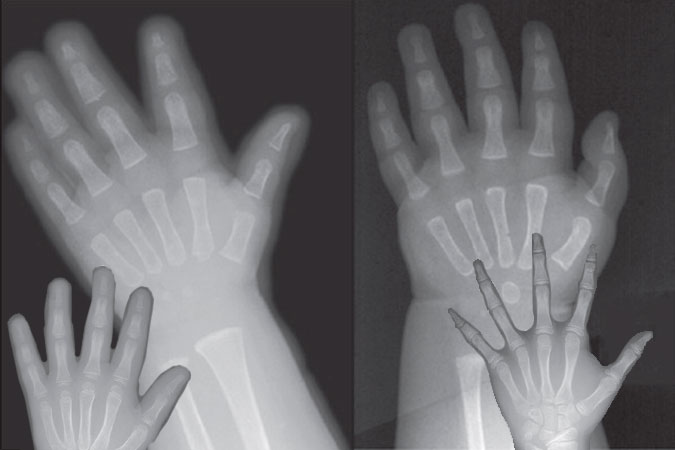
Skeletal Age Determination
Throughout the course of our lives, our bones undergo a systematic and predictable series of changes and developments, transforming from the soft, malleable structures present in infancy into the rigid, supportive framework that characterizes the adult human body. The timeline for this transformative process – which culminates in what is referred to as ‘skeletal maturity’ – generally ranges between 20 and 25 years in western countries, although variances may occur due to factors such as geographic location, socioeconomic conditions, genetic influences, and certain disease states. The determination of an individual’s skeletal age forms a crucial part of various medical evaluations and treatments.
Understanding Skeletal Maturity
From birth to skeletal maturity, bony growth and development occur in an orderly and predictable manner. The chronological age of an individual often aligns with their skeletal age in healthy conditions, making skeletal age an accurate representation of their actual age. This match is vital for not only medical evaluation but also legal proceedings, offering a precise and objective method to establish the age of an individual.
Skeletal maturity is primarily determined by radiographic evaluation of bones, most commonly the nondominant (often left) hand. This bone is typically x-rayed, and the resulting image is juxtaposed against a series of standard radiographs. Through this comparison, healthcare professionals can estimate the skeletal age of the patient. Alternative imaging methods, such as ultrasound or MRI scans, may also be used, providing comprehensive information about the bone’s development and maturation stage.
The Role of Genetics and Socioeconomic Conditions
The timing and progression of skeletal maturity are influenced by various factors. For instance, genetic traits play a substantial role in determining the rate of bone growth and the eventual attainment of skeletal maturity. Certain inherited conditions can lead to either accelerated or delayed bone development.
Geographic location and socioeconomic conditions, too, are significant contributors to skeletal maturity. In developing regions, where malnutrition and inadequate healthcare are more prevalent, skeletal maturity might occur later than in more affluent regions. Prolonged malnutrition, especially during the formative years of life, can slow bone growth, resulting in a delay in skeletal maturity.
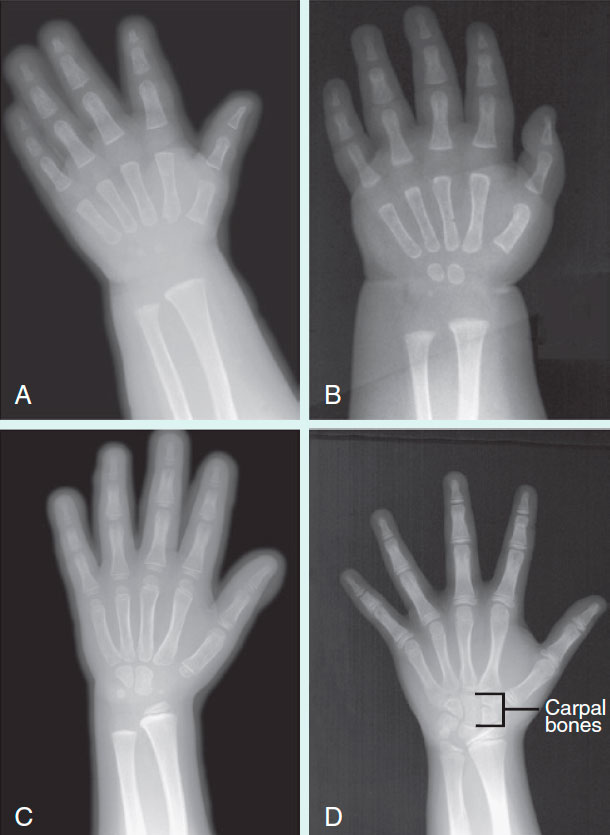
Skeletal Age in Disease States
Certain disease states, such as hypothyroidism and malnutrition, can cause a significant lag in bony maturity. Hypothyroidism, for example, can slow metabolic processes and, in turn, inhibit bone development. Similarly, malnutrition leads to insufficient nutrient supply for normal growth processes, causing a slowdown in skeletal maturation. In these instances, the skeletal age of the patient may be significantly lower than their chronological age, indicating a need for medical intervention.
In such cases, an accurate determination of skeletal age allows healthcare professionals to identify the discrepancy between the patient’s skeletal and chronological ages. This recognition can lead to more tailored treatment plans and interventions, contributing to improved health outcomes.
Conclusion
The determination of skeletal age, therefore, is a vital tool in modern medicine. It aids in accurately understanding an individual’s physical maturation level, informing treatment plans, and providing essential evidence in legal cases. As we continue to refine our understanding of bone growth and development, the accuracy and utility of skeletal age determination will only increase, further enhancing its value in a clinical and legal context.











